Can you have varicose veins removed?
There are many reasons why people may want to have varicose veins removed. Some people may feel self-conscious about how they look, while others may be experiencing pain or other problems caused by the veins. In either case, there are a variety of treatment options available.
One of the most common varicose vein removal methods is ambulatory phlebectomy. This procedure involves making small incisions on the skin’s surface and using a special hook-like instrument to remove the veins. This method is effective in removing superficial varicose veins, i.e., the bulging and visible varicose veins, and it has a relatively low risk of complications. Ambulatory phlebectomy is purely cosmetic because it can’t treat chronic venous insufficiency, which is the root cause of most vein problems.
Endovenous laser ablation and radiofrequency ablation are two other minimally invasive treatment options that can treat the root cause of varicose veins and prevent them from returning. These procedures involve using heat to destroy the vein. Endovenous ablation involves inserting a catheter into the diseased vein under ultrasound guidance, following which laser energy or thermal energy is released to destroy the diseased vein. The accumulated blood reroutes into healthier leg veins, thus restoring optimal blood circulation.
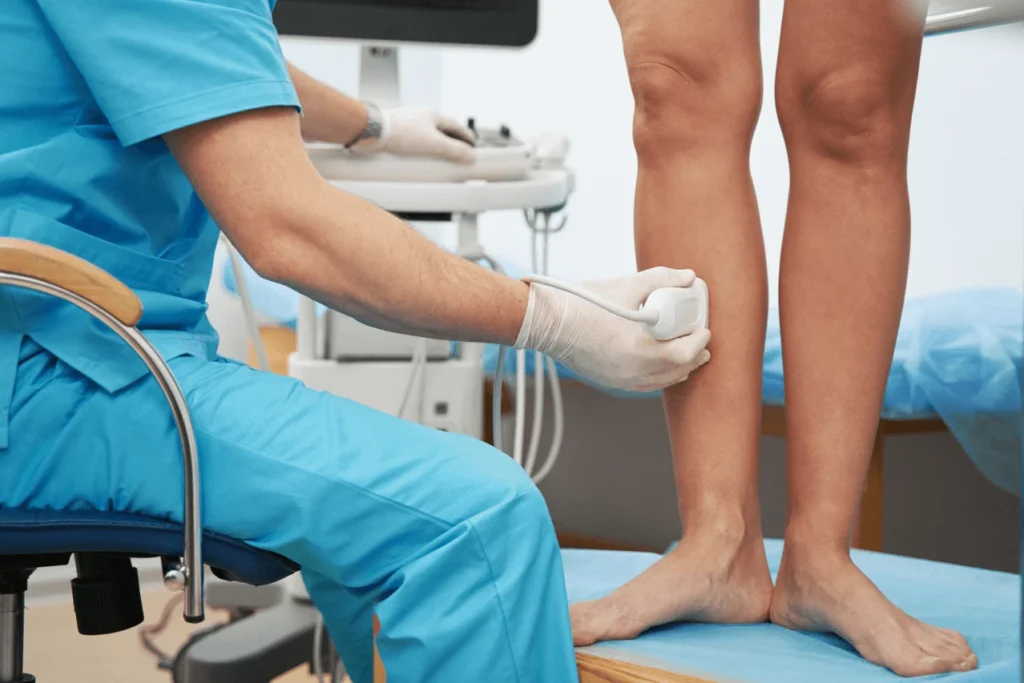
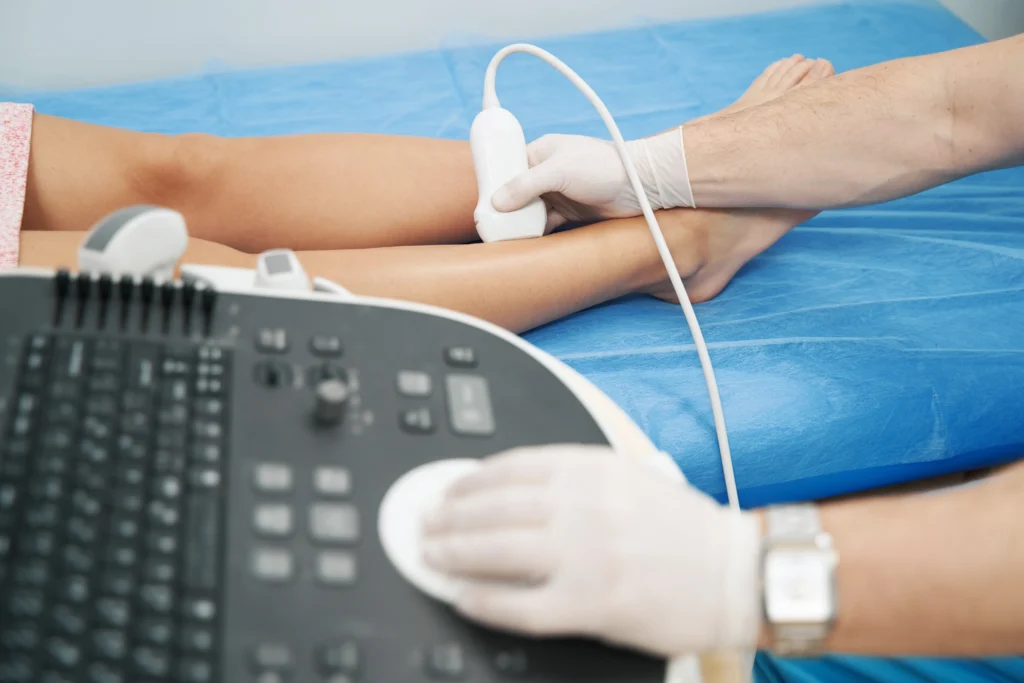
Your vein doctor may perform a doppler ultrasound to help plan the best way to remove your varicose veins. During a doppler ultrasound, the vein doctor channels sonic waves into your legs to produce a visual of the blood flow in your leg veins. This procedure helps the vein doctor diagnose underlying chronic venous insufficiency and curate a personalized vein treatment plan. If you’re in or around the National Capital Region, you can find our board-certified vein doctors at 10215 Fernwood Rd, Suite 301, Bethesda.
Please schedule an appointment at our vein clinics in Maryland.

What are the signs of a blood clot after vein ablation?
If you’ve had a vein ablation, it’s important to know the signs of blood clotting. While the procedure is generally safe, there is always a risk of complications. A blood clot can occur in the vein that was treated or in a nearby vein. If a blood clot forms, it can block the flow of blood and cause serious problems.
The most common symptom of a blood clot after vein ablation is pain. This can be a dull ache or a more sharp, localized pain. You may also experience swelling, redness, and warmth in the affected area. If the clot is in your leg, you may also have difficulty walking. If you experience any of these symptoms, you must contact your vein doctor right away.
Vein ablation is a safe and effective treatment for varicose veins with a negligible risk of complications and a nearly perfect success rate. However, like all procedures, there are risks involved. Talk to your vein doctor about the risks before having the procedure done.
Can varicose veins be permanently removed?
Bulging, twisted veins are a pain—literally and figuratively. They cause throbbing, burning, and itching, and they can also lead to serious medical problems, like blood clots. If you’re dealing with varicose veins, the good news is that several treatment options are available to help improve the appearance of your legs and reduce your discomfort. But what about permanently getting rid of varicose veins? Is that even possible?
Unfortunately, there is no one-size-fits-all answer to this question. While several treatments can effectively improve the appearance of varicose veins and reduce symptoms, there is no guaranteed way to permanently eliminate them. Minimally invasive vein treatments, such as endovenous ablation, ambulatory phlebectomy, and radiofrequency ablation, can remove superficial varicose veins and treat underlying vein disease. Once your varicose veins are removed, they can’t return.
But you can still develop new varicose veins. Patients with a history of vein problems have a high risk of vein disease recurrence. And the risk can be further increased because of age, pregnancy, injuries, prolonged periods of sitting or standing, and other factors.
That said, there are a few things you can do to help minimize your risk of developing varicose veins in the first place. First, avoid sitting or standing for long periods of time. If you must stand for long periods, try to move around as much as possible to keep the blood flowing. Secondly, exercise regularly. This will improve circulation and prevent the pooling of blood in the veins. Finally, wear compression stockings to improve blood circulation.
Should I get my varicose veins treated?
If you have varicose veins, you may have heard that treatment is not necessary. After all, varicose veins are not dangerous, right? Wrong. While varicose veins may not be immediately life-threatening, they can cause serious problems if left untreated. Here are some potential complications of varicose veins:
- Leg Ulcers: Also called stasis ulcers, these occur when blood flow in the veins is slowed or halted. This can cause the skin to break down, leading to painful open sores.
- Blood Clots: When blood flow is slowed, it can lead to blood clots. If a clot forms in the veins of the leg, it’s called deep vein thrombosis (DVT). This can be a serious condition because the clot can break loose and travel to the lungs, causing a pulmonary embolism.
- Skin Changes: Varicose veins can cause the skin around the veins to thin and turn a dark color. The lack of effective blood flow in the legs can also lead to skin discoloration.